 |
|

Sleeping Sickness
[Human African Trypanosomiasis-HAT]
[Human African Trypanosomiasis-HAT]
60 million people at risk in sub-Saharan Africa
 What is the annual impact of HAT?
What is the annual impact of HAT?50,000-70,000 cases(1)
1,525,000 DALYs(2) (3)
Large proportions of communities can be affected by HAT, with serious social and economic consequences. Epidemics at the end of the 20th century infected up to 50% of population in several villages across rural Africa.
Where does HAT occur?
Of the 36 countries considered endemic for HAT, the 7 most affected countries represent 97% of all reported cases (see map).
The Democratic Republic of the Congo (DRC) alone accounts for 2/3 of reported cases (4). HAT primarily occurs in the poorest, most rural areas in Africa, where difficulty of diagnosis, political instability, and lack of health surveillance make estimates of disease prevalence difficult to ascertain.
 How is HAT transmitted?
How is HAT transmitted?Transmitted to humans by tsetse flies, HAT is caused by two sub-species of the
kinetoplastid protozoan parasite, Trypanosoma brucei: T. b. gambiense (west African), T. b. rhodensiense (east African).
What are the symptoms/presentations?
HAT occurs in two stages:
• stage 1 - the haemolymphatic phase – includes non-specific symptoms like headaches
and bouts of fever (generally goes undiagnosed without active HAT surveillance ).
• stage 2 - the later, neurologic phase – occurs when the parasite crosses the bloodbrain barrier (BBB) and can lead to serious sleep cycle disruptions, paralysis, progressive mental deterioration, with behaviourial changes, and, ultimately, results in death without effective treatment.
What are the Current Therapies for Stage 2?
Melarsoprol: High toxicity, rising rates of treatment failure, still received by the majority of stage 2 patients in 2007
Introduced in the 1940s, this organo-arsenic drug has remained the mainstay treatment for stage 2 HAT, despite its high toxicity (5-6% mortality following treatment, mainly due to reactive encephalopathy). Treatment failure rates are being reported at increasing rates, up to 50% in some regions.
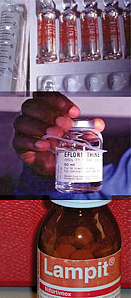
Eflornithine (DFMO): Relatively well tolerated, efficacious, but resource-intensive; received by ~30% of patients in 2007
During the 1980s, this anti-cancer was assessed as trypanostatic drug for sleeping sickness and was registered at the FDA for stage 2 T. b. gambiense HAT in 1989. Recent experience with eflornithine as first-line treatment has demonstrated that it is safer than melarsoprol, and with good efficacy. Its widespread use, particularly in resource-poor settings, is greatly limited by the impracticality of its administration: repeated slow intravenous infusions, given every six hours, twice a day for 14 consecutive days, are required, which requires nursing staff, medical supervision, and large amounts of extra materials (e.g. infusion fluids, infusions sets, sterile gauze). Over the past five years, only 15% of stage 2 HAT Patients had access to this treatment, but its use is now gradually increasing to 30% for 2007 thanks to the distribution by WHO of eflornithine in kits (including all equipment and associated training).
Nifurtimox: Cheap, easy to use, but limited efficacy in monotherapy & not registered for HAT
This oral trypanocidal drug, licensed for Chagas disease, has been used on a compassionate basis for treatment for stage 2 HAT, but has insufficient efficacy for use as a monotherapy for this fatal disease.
1- World Health Organization (WHO). Wkly Epidemiol Rec. 2006:81;71-80.
2 - WHO. The World Health Report. Geneva; 2004. Available from http://www.who.int/whr/2004. Accessed Aug 12, 2008.
3 - DALYs are a measure of societal impact, being the sum of years of potential life lost due to premature mortality and the years of productive life lost due to disability.
4 - Simarro PP, Jannin J, Cattand P. PLoS Med. 2008;5:e55.
Introduced in the 1940s, this organo-arsenic drug has remained the mainstay treatment for stage 2 HAT, despite its high toxicity (5-6% mortality following treatment, mainly due to reactive encephalopathy). Treatment failure rates are being reported at increasing rates, up to 50% in some regions.
Eflornithine (DFMO): Relatively well tolerated, efficacious, but resource-intensive; received by ~30% of patients in 2007
During the 1980s, this anti-cancer was assessed as trypanostatic drug for sleeping sickness and was registered at the FDA for stage 2 T. b. gambiense HAT in 1989. Recent experience with eflornithine as first-line treatment has demonstrated that it is safer than melarsoprol, and with good efficacy. Its widespread use, particularly in resource-poor settings, is greatly limited by the impracticality of its administration: repeated slow intravenous infusions, given every six hours, twice a day for 14 consecutive days, are required, which requires nursing staff, medical supervision, and large amounts of extra materials (e.g. infusion fluids, infusions sets, sterile gauze). Over the past five years, only 15% of stage 2 HAT Patients had access to this treatment, but its use is now gradually increasing to 30% for 2007 thanks to the distribution by WHO of eflornithine in kits (including all equipment and associated training).
Nifurtimox: Cheap, easy to use, but limited efficacy in monotherapy & not registered for HAT
This oral trypanocidal drug, licensed for Chagas disease, has been used on a compassionate basis for treatment for stage 2 HAT, but has insufficient efficacy for use as a monotherapy for this fatal disease.
1- World Health Organization (WHO). Wkly Epidemiol Rec. 2006:81;71-80.
2 - WHO. The World Health Report. Geneva; 2004. Available from http://www.who.int/whr/2004. Accessed Aug 12, 2008.
3 - DALYs are a measure of societal impact, being the sum of years of potential life lost due to premature mortality and the years of productive life lost due to disability.
4 - Simarro PP, Jannin J, Cattand P. PLoS Med. 2008;5:e55.
Published by Drugs for Neglected Diseases Initiative - 15 Chemin Louis-Dunant 1202 Geneva Switzerland - Photo credits: DNDi unless otherwise stated - Editor: Sadia Kaenzig - Tel: +41 22 906 9230 - Fax: +41 22 906 9231 - www.DNDi.org